Author: Mr Oliver Eaton BSc (Hons), PG.Cert – Orthopaedic Specialist
Reviewed by: Mr William Sharples BSc (Hons) – Pain Management Expert
Last Updated: September 2025
In this article, you will find out everything you need to know about cluster headaches and the most effective ways to treat them, including an advanced treatment called prolotherapy.
Table of Contents
- Uncovering the Causes of Cluster Headaches
- Cluster Headache Symptoms and Types
- Diagnosis and Misdiagnosis of Cluster Headaches
- Treatment Options for Cluster Headaches
- Lifestyle Changes and Alternative Therapies
- Prolotherapy
- Coping with Cluster Headaches: Support and Resources
- Summary
- Frequently Asked Questions
- Contact ProHealth Clinic
- Author Bio
- References
Uncovering the Causes of Cluster Headaches
Cluster headaches are complex and can be triggered by a combination of brain activity (especially hypothalamus dysfunction), genetic predisposition, and environmental factors. The hypothalamus, which regulates circadian rhythms, is thought to play a key role—explaining why attacks often occur at the same time each day. Genetics also matter: having a first-degree relative with cluster headaches increases your risk. Environmental triggers include smoking, alcohol, strong odors, changes in sleep, stress, and certain foods (like those with nitrates).
Brain Activity and Hypothalamus Dysfunction
The hypothalamus helps regulate sleep and body rhythms. Dysfunction here is linked to the timing and severity of cluster headaches, which often wake sufferers at night or early morning.
Genetic Factors
Cluster headaches can run in families. Genes related to circadian rhythms and sleep-wake cycles (like PER3 and orexin-B) are implicated. If a close relative has cluster headaches, your risk is higher.
Environmental Triggers
Smoking, alcohol, bright lights, high temperatures, stress, and poor sleep are common triggers. Avoiding these can help reduce attack frequency.
Cluster Headache Symptoms and Types
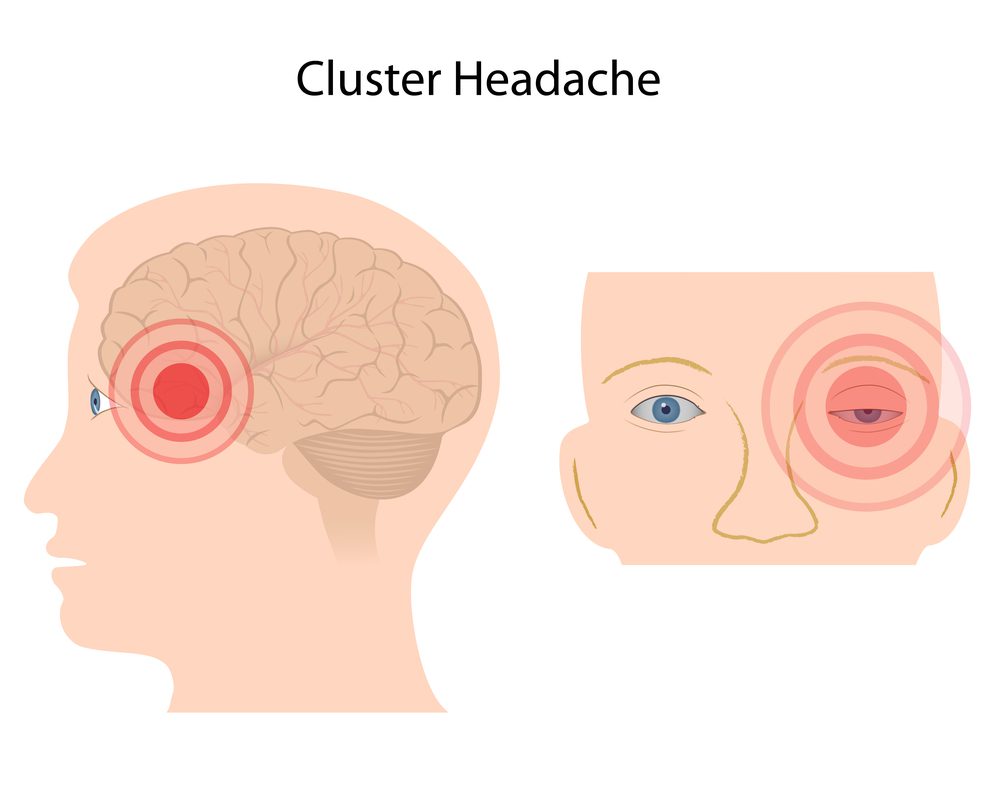
Cluster headaches cause severe, one-sided pain (often around or behind the eye) lasting 15–180 minutes. Attacks may occur several times a day, often at the same time. Symptoms include:
- Red, watery eye
- Nasal congestion or runny nose
- Eyelid drooping or swelling
- Facial sweating
There are two main types:
- Episodic: Attacks occur in periods (weeks to months) with remission in between.
- Chronic: Attacks occur year-round with little or no remission.
Diagnosis and Misdiagnosis of Cluster Headaches
Diagnosis is based on ICHD-3 criteria: severe, unilateral pain with autonomic symptoms, lasting 15–180 minutes, and occurring up to 8 times a day. Misdiagnosis is common—cluster headaches are often mistaken for migraines, sinus headaches, or trigeminal neuralgia. Keeping a headache diary can help. Accurate diagnosis is crucial for effective treatment.
Treatment Options for Cluster Headaches
Treatment aims to relieve acute attacks and prevent future ones. Acute relief includes 100% oxygen therapy and nonoral triptans (like sumatriptan). Preventive medications include verapamil, lithium, and corticosteroids. For chronic cases, nerve blocks or neuromodulation (like occipital nerve stimulation) may be considered.
Lifestyle Changes and Alternative Therapies
Avoiding triggers (alcohol, smoking, certain foods, bright lights, heat, and stress) is key. Maintain regular sleep, manage stress, and stay hydrated. Melatonin supplements, capsaicin nasal spray, and transcutaneous vagus nerve stimulation are alternative options that may help some people.
Prolotherapy
In recent years, Prolotherapy has built its reputation within the medical community for its clinically proven ability to treat cluster headaches.
Published research has proven its pain-relieving, anti-inflammatory and regenerative benefits.
Prolotherapy involves injecting a natural regenerative solution with tiny needles. This has been shown to stimulate the production of collagen cells, the small cells needed to help with cluster headaches.
As prolotherapy is helping to treat the root cause of cluster headaches, it is deemed to be a permanent fix, preventing the symptoms from returning.

Coping with Cluster Headaches: Support and Resources
Support groups, counseling, and online resources (like O.U.C.H.) can help you manage the emotional and practical challenges of cluster headaches. Sharing experiences and learning from others can reduce isolation and improve coping.
Summary
Cluster headaches are severe, complex, and often misunderstood. Understanding your triggers, getting an accurate diagnosis, and using a combination of medical, lifestyle, and alternative therapies can help you manage attacks and improve your quality of life. Prolotherapy offers a promising, regenerative option for long-term relief.
Frequently Asked Questions
What is a cluster headache caused from?
Cluster headaches are linked to hypothalamus dysfunction, genetic factors, and environmental triggers like smoking and alcohol. The exact cause is not fully understood.
How do you stop a cluster headache?
High-flow oxygen therapy and sumatriptan nasal spray or injection are the fastest ways to stop an attack.
Are cluster headaches caused by stress?
Stress is not a direct cause, but it can trigger attacks in some people.
Who is most likely to suffer from cluster headaches?
Men, especially those with a family history of migraines or cluster headaches, are most at risk.
How are cluster headaches diagnosed?
Diagnosis is based on ICHD-3 criteria: severe, one-sided pain, autonomic symptoms, and attack frequency/duration.
Contact ProHealth Clinic Today for Your FREE 15-Minute Discovery Call
Don’t let cluster headaches control your life any longer. Join the thousands of patients who have found lasting relief through prolotherapy at ProHealth Clinic.
Get in Touch
- Phone: +44 1234 380345
- Email: info@prohealthclinic.co.uk
Our Clinic Locations
- London: 104 Harley Street, Marylebone, W1G 7JD
- Manchester: The Hadley Clinic, 64 Bridge Street, M3 3BN
- Bedford: The Village Medical Centre, Kingswood Way, MK40 4GH
All clinics offer the same award-winning prolotherapy treatment with convenient appointment times, including evenings and weekends.
Author Bio
Having performed over 10,000 procedures, Mr Oliver Eaton is one of the UK’s leading practitioners in the field of treating cluster headaches, with patients travelling to see him from across the UK, Europe, and the Middle East.
With over 12 years of clinical experience, Oliver is dedicated to helping patients understand their symptoms associated with cluster headaches and providing effective treatment options to alleviate them.
He qualified in Prolozone Therapy and Prolotherapy in America with the American Academy of Ozonotherapy. He continued on to complete further qualifications at the Royal Society of Medicine, Charing Cross Hospital in London, Keele University’s Anatomy & Surgical Training Centre, and the medical department of Heidelberg University in Germany.
Over the years he has had the privilege of treating many elite-level athletes, including both Olympic and Commonwealth medallists.
Mr Eaton’s expertise has been featured in many national news and media publications, including The Telegraph, The Daily Mail, The Daily Express, Women’s Health Magazine, and The Scotsman.
Connect with Oliver Eaton on LinkedIn
References
- Kandel SA, Mandiga P. Cluster Headache. StatPearls [Internet]. 2022. View Resource
- Wei DY, Ong JJ, Goadsby PJ. Cluster headache: epidemiology, pathophysiology, clinical features, and diagnosis. Ann Indian Acad Neurol. 2018;21(Suppl 1):S3.
- Ljubisavljevic S, Zidverc Trajkovic J. Cluster headache: pathophysiology, diagnosis and treatment. J Neurol. 2019;266(5):1059-1066.
- Gaul C, Diener HC, Müller OM. Cluster headache: clinical features and therapeutic options. Dtsch Arztebl Int. 2011;108(33):543.
- Sohn JH, Choi YJ, Kim BK, et al. Clinical Features of Probable Cluster Headache: A Prospective, Cross-Sectional Multicenter Study. Front Neurol. 2018;9:908. View Study
- Hoffmann J, May A. Diagnosis, pathophysiology, and management of cluster headache. Lancet Neurol. 2018;17(1):75-83.
- Edvinsson L, Goadsby PJ. Neuropeptides in migraine and cluster headache. Cephalalgia. 1994;14(5):320-327.
- Steinberg A, Nilsson Remahl AIM. Role of nitric oxide in cluster headache. Curr Pain Headache Rep. 2012;16(2):185-190.
- Holle D, Obermann M. Cluster headache and the hypothalamus: causal relationship or epiphenomenon? Expert Rev Neurother. 2011;11(9):1255-1263.
- Petersen AS, Barloese MC, Jensen RH. Oxygen treatment of cluster headache: a review. Cephalalgia. 2014;34(13):1079-1087.
- Nowacki A, Moir L, Owen SL, et al. Deep brain stimulation of chronic cluster headaches: Posterior hypothalamus, ventral tegmentum and beyond. Cephalalgia. 2019;39(9):1111-1120.
Disclaimer: This article is for informational purposes only and does not substitute for professional medical advice. Always consult your healthcare provider before making treatment decisions.