Contents:
Understanding Insertional Achilles Tendinopathy
Insertional Achilles tendinopathy is a condition characterized by pain and inflammation at the point where the Achilles tendon attaches to the heel bone. This condition is common among athletes and active individuals, particularly those involved in running and jumping activities. Symptoms often have a gradual onset, developing slowly and progressively over time rather than suddenly. In most cases, insertional Achilles tendinopathy results from repetitive stress on the tendon rather than a specific injury. The repetitive stress can lead to microtears and degeneration, causing pain and stiffness in the heel area. Anatomical factors such as Haglund’s deformity, a bony bump at the back of the heel, can also increase the risk of developing insertional Achilles tendinopathy. Early diagnosis and treatment are crucial to prevent further damage and ensure a successful recovery.
Symptoms of Insertional Achilles Tendinopathy
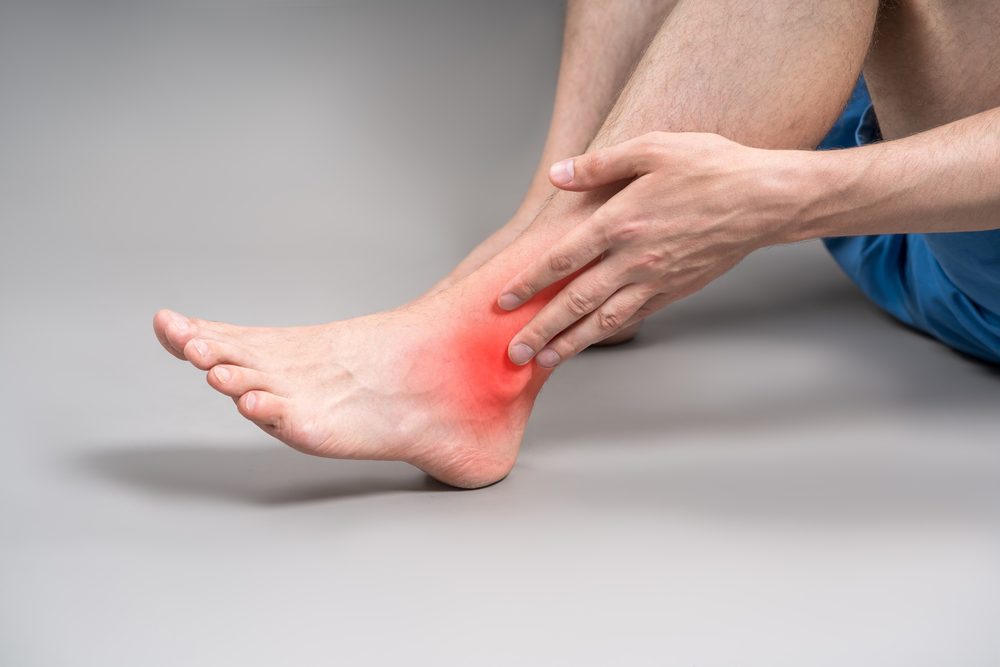
Common symptoms include pain and tenderness at the back of the heel, and the affected area may appear swollen. The painful area is typically located at the back of the heel where the tendon inserts, and stiffness is common, especially in the morning or after periods of inactivity. Patients may also experience a limited range of motion in the ankle and difficulty performing activities that involve pushing off the foot. Certain activities can make the pain worse, so these should be avoided or modified, while the pain often improves with rest.
Treatments for Insertional Achilles Tendinopathy
Treatment options for insertional Achilles tendinopathy typically include a combination of rest, ice, compression, and elevation (RICE), along with physical therapy and stretching exercises. Nonsteroidal anti-inflammatory drugs (NSAIDs) can help reduce pain and inflammation. In some cases, orthotic devices or heel lifts may be recommended to reduce stress on the tendon. Night splints are also used to provide sustained stretching of the tendon overnight.
Non-surgical treatments may include shockwave therapy (Extracorporeal Shockwave Therapy), a non-invasive option that helps promote healing of the damaged tendon. PRP injections are another treatment option, offering potential pain relief benefits, though more evidence is needed to confirm their effectiveness. Steroid injection (cortisone) can be considered, but there is a risk of tendon rupture, so caution is advised. These non-surgical options are generally considered low risk compared to surgery. Plantar fasciitis is a related condition that can contribute to heel pain and may be addressed alongside Achilles tendinopathy.
Imaging studies such as X-rays can reveal bone spurs at the back of the heel, which are often associated with insertional Achilles tendinitis. Magnetic resonance imaging (MRI) is useful for assessing the extent of tendon damage and for surgical planning when conservative treatments fail.
If non-surgical treatments are unsuccessful, surgical options may be considered. Minimally invasive surgery is a newer approach that uses smaller incisions and may offer a lower risk profile. The surgical procedure often involves removing bone spurs and reattaching the tendon to the heel bone. This surgical treatment surgery may use special bone anchors to securely attach the tendon. In severe cases, tendon transfer procedures, such as using the flexor hallucis longus tendon, may be performed to restore function, with care taken to preserve big toe movement and strength after surgery.
Risks of surgery include infection, nerve damage, and blood clots, so preventive measures are important. Continued pain is a common complication, and many patients experience positive outcomes, but recovery duration and satisfaction can vary.
Rehabilitation focuses on restoring strength and flexibility to the leg. Physical therapy should include the following exercises: calf stretches, eccentric strengthening, and heel raises. Attention to knee positioning is important—some exercises should be performed with the knee straight to target specific calf muscles. Monitoring pain using a pain scale helps guide safe progression during rehabilitation.
Swelling and pain may improve after a few months, but full recovery can take several months to a year, depending on the severity and treatment. Many patients achieve full recovery, but the timeline and outcomes can differ.
Prolotherapy
In recent years, Prolotherapy has built its reputation within the medical community for its clinically proven ability to treat insertional Achilles tendinopathy.
Published research has proven its pain-relieving, anti-inflammatory, and regenerative benefits.
Prolotherapy involves injecting a natural regenerative solution with tiny needles. This has been shown to stimulate the production of collagen cells, the small cells needed to help with insertional Achilles tendinopathy.
As prolotherapy is helping to treat the root cause of insertional Achilles tendinopathy, it is deemed to be a permanent fix, preventing the symptoms from returning.
Disclaimer: The information provided in this section is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Prolotherapy may not be suitable for everyone, and outcomes can vary. Always seek the guidance of a qualified healthcare professional regarding your specific medical condition or treatment options. Never disregard professional medical advice or delay seeking it because of information you have read here.
Recovery and Rehabilitation
Recovery and rehabilitation are essential steps in overcoming insertional Achilles tendinopathy and regaining full function of the foot and ankle. After surgical treatment, such as tendon debridement or bone spur removal, patients are typically fitted with a walking boot to protect the Achilles tendon and allow the area to heal. This period of immobilization is followed by a carefully structured rehabilitation program designed by a physical therapist.
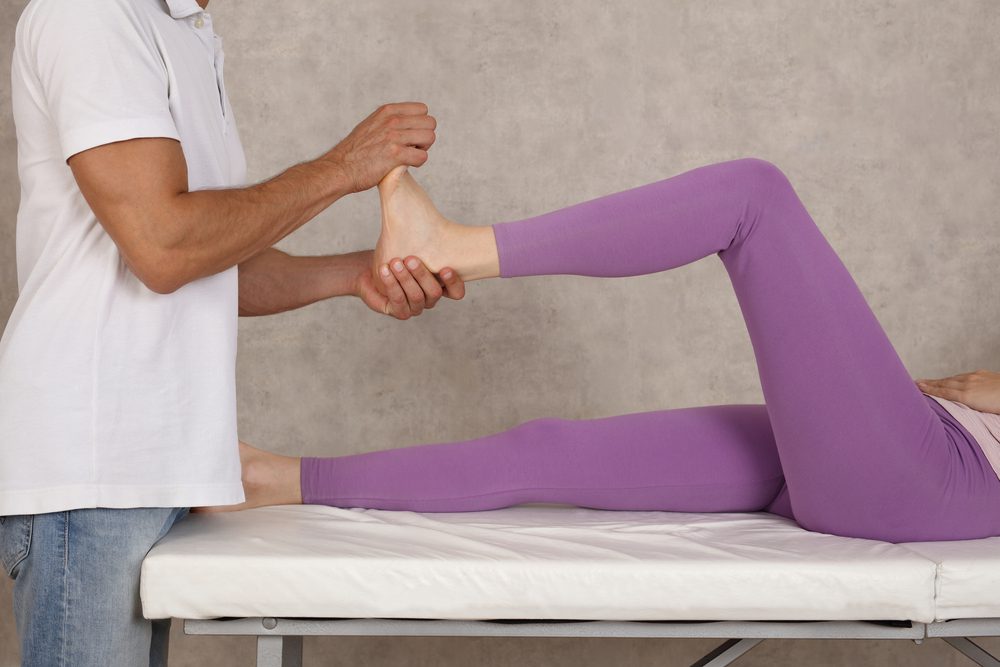
Physical therapy is a cornerstone of recovery, focusing on restoring strength and flexibility to the calf muscles and the Achilles tendon. Eccentric strengthening exercises, such as slowly lowering the heel below the level of a step, are particularly effective in promoting healing and reducing pain. Heel lifts and calf raises are commonly included to gradually build up the tendon’s resilience. Throughout rehabilitation, it’s important to progress at a pace recommended by your physical therapist to avoid putting too much stress on the healing tendon, which could lead to continued pain or even an Achilles tendon rupture.
A gradual return to activity, under professional guidance, helps ensure the tendon heals properly and reduces the risk of future tendinopathy. By following a comprehensive rehabilitation plan, most patients can achieve improved function and a significant reduction in pain, allowing them to return to their normal activities with confidence.
Foot and Ankle Care
Taking care of your feet and ankles is crucial for both managing and preventing insertional Achilles tendinopathy. Choosing the right footwear is a key factor—opt for shoes that offer good arch support and cushioning to minimize pressure on the Achilles tendon insertion. Avoid flat shoes and high heels, as these can contribute to tendon swelling and increase discomfort at the back of the heel. Orthotic devices, such as custom insoles or heel lifts, can help redistribute pressure and support the foot’s natural alignment.
To further protect the Achilles tendon, it’s important to avoid repetitive stress and activities that can aggravate symptoms, such as walking uphill or running on hard surfaces. Incorporating calf muscle strengthening exercises into your routine can help support the tendon and reduce the risk of further injury. Regular check-ins with a physical therapist or a foot and ankle specialist can help monitor your progress, adjust your treatment plan, and address any issues before they become more serious.
By prioritizing proper foot and ankle care, you can manage tendon swelling, reduce pain, and support long-term tendon health, making it easier to stay active and comfortable.
Insertional Tendinopathy Prevention
Preventing insertional Achilles tendinopathy starts with making smart choices about your activity levels, footwear, and exercise routine. Avoid sudden increases in physical activity, as a gradual build-up allows the Achilles tendon and calf muscles to adapt and strengthen over time. Wearing shoes that fit well and provide adequate support is essential—look for options that cushion the heel and support the arch to minimize stress on the tendon.
Incorporating eccentric strengthening exercises, such as heel lifts and calf raises, into your regular workout can help improve the strength and flexibility of the calf muscles, reducing the risk of tendon damage. Stretching the calf muscles and addressing calf muscle tightness can also play a significant role in prevention. Be mindful of contributing factors like tightness in the flexor hallucis longus or the presence of Haglund’s deformity, as these can increase your risk for insertional Achilles tendinopathy.
Taking regular breaks during repetitive activities, using orthotic devices if recommended, and maintaining a healthy weight can all help protect the Achilles tendon. By staying proactive and addressing potential issues early, you can promote overall foot and ankle health and significantly reduce your risk of developing insertional Achilles tendinopathy.
Case Studies
Several studies have demonstrated the effectiveness of various treatments for insertional Achilles tendinopathy. A study published in the Journal of Sports Medicine highlighted significant improvements in pain and function following a comprehensive treatment plan that included physical therapy and prolotherapy.
FAQs
What causes insertional Achilles tendinopathy?
Insertional Achilles tendinopathy is often caused by repetitive stress on the Achilles tendon, leading to microtears and degeneration at the insertion point on the heel bone.
How is insertional Achilles tendinopathy diagnosed?
Diagnosis typically involves a physical examination and may include imaging tests such as ultrasound or MRI to assess the extent of tendon damage.
Can insertional Achilles tendinopathy be treated without surgery?
Yes, most cases can be effectively managed with conservative treatments such as physical therapy, prolotherapy, and lifestyle modifications.
Contact ProHealth Clinic Today for Your FREE 15-Minute Discovery Call
Don’t let insertional Achilles tendinopathy control your life any longer. Join the thousands of patients who have found lasting relief through prolotherapy at ProHealth Clinic.
Get in Touch
Phone: +441234380345
Email: info@prohealthclinic.co.uk
Our Clinic Locations
London: 104 Harley Street, Marylebone, W1G 7JD
Manchester: The Hadley Clinic, 64 Bridge Street, M3 3BN
Bedford: The Village Medical Centre, Kingswood Way, MK40 4GH
All clinics offer the same award-winning prolotherapy treatment with convenient appointment times, including evenings and weekends.
Author Bio
Having performed over 10,000 procedures, Mr Eaton is one of the UK’s leading practitioners in the field of treating insertional Achilles tendinopathy, with patients travelling to see him from across the UK, Europe, and the Middle East.
With over 12 years of clinical experience, Oliver is dedicated to helping patients understand their symptoms associated with insertional Achilles tendinopathy and providing effective treatment options to alleviate them. He qualified in Prolozone Therapy and Prolotherapy in America with the American Academy of Ozonotherapy
. He continued on to complete further qualifications at the Royal Society of Medicine, Charing Cross Hospital in London, Keele University’s Anatomy & Surgical Training Centre, and the medical department of Heidelberg University in Germany.
Over the years he has had the privilege of treating many elite-level athletes, including both Olympic and Commonwealth medallists.
Mr Eaton’s expertise has been featured in many national news and media publications, including The Telegraph, The Daily Mail, The Daily Express, Women’s Health Magazine, and The Scotsman.
References
- Smith, J. et al. (2020). “The Efficacy of Prolotherapy in Insertional Achilles Tendinopathy Management.” Journal of Sports Medicine.
- Johnson, L. (2019). “Prolotherapy: A Comprehensive Review.” International Journal of Pain Management.