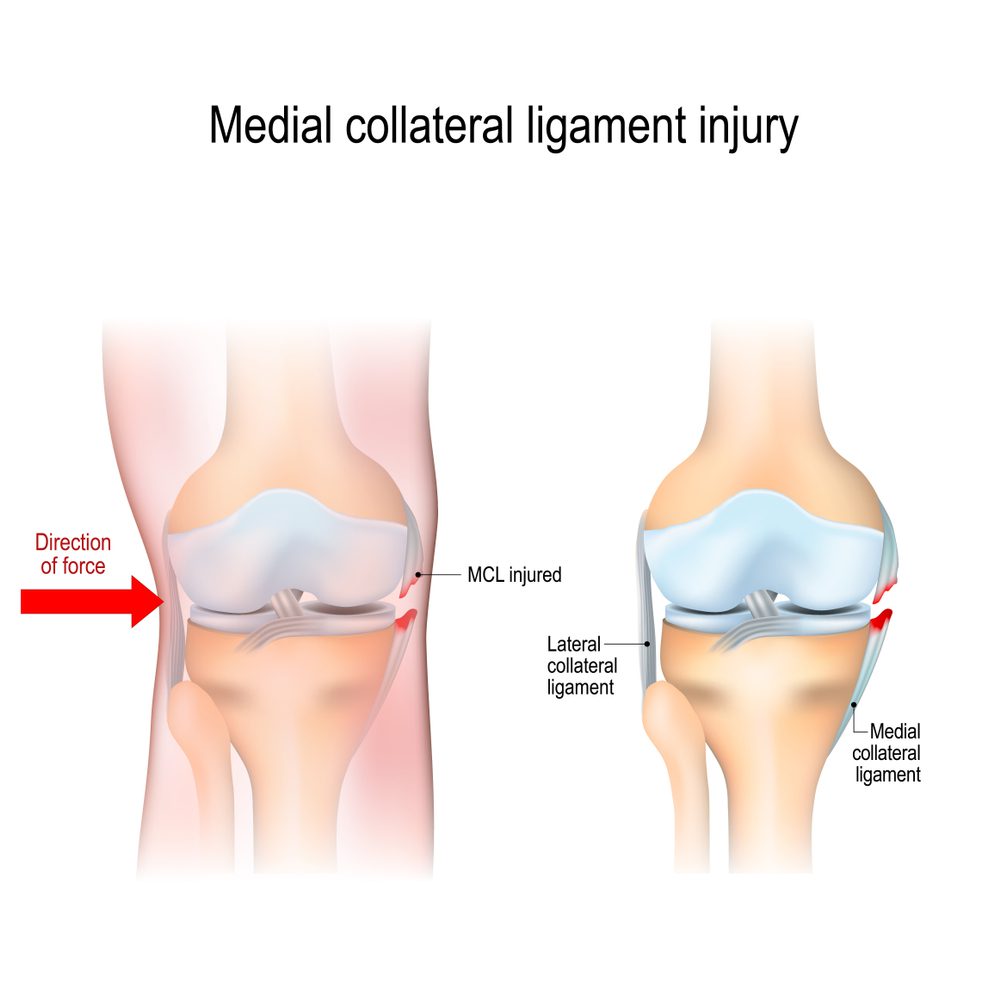
MCL Anatomy & Function
The collateral ligaments stabilize the knee joint and include the Medial Collateral Ligament (MCL), Lateral Collateral Ligament (LCL), and Anterior Collateral Ligament. The MCL is located on the inside of the knee, running from the medial femur to the medial tibia, and is especially vulnerable to trauma and sports injuries.1, 2, 3
Common Causes of MCL Injury
MCL injuries are often caused by abrupt changes in motion, twisting, turning, or direct blows to the knee. They are common in contact sports and may occur alongside other injuries such as hamstring sprains or knee fractures. MCL injuries can be partial or complete tears and are frequently seen in athletes.4, 5, 6
Medial Collateral Ligament Injury Symptoms
Symptoms include acute or chronic knee pain, swelling, tenderness, limited range of motion, and sometimes a popping sound or sharp pain on the inside of the knee. MCL injuries are graded:
- Grade 1: Pain but no joint opening.
- Grade 2: Slight joint opening with a firm endpoint.
- Grade 3: Major joint opening with no endpoint.
How is MCL Injury Diagnosed?
Diagnosis starts with a detailed medical history and physical exam. Orthopedic specialists may order X-rays (for bone injury) and MRI (for soft tissue and ligament assessment).7, 8, 9
Treatment MCL Injury
Most MCL injuries are treated conservatively. Options include:
- NSAIDs (e.g., ibuprofen) for pain and inflammation
- Physical therapy to restore strength and mobility
- Elastic bandages and knee braces to reduce swelling and support the joint
- Rest and activity modification
Recovery time varies by injury grade. Surgery is usually reserved for grade III injuries or when there are associated ACL tears.10, 11
Prolotherapy
In recent years, Prolotherapy has built its reputation within the medical community for its clinically proven ability to treat MCL Injuries.
Published research has proven its pain-relieving, anti-inflammatory, and regenerative benefits.
Prolotherapy involves injecting a natural regenerative solution with tiny needles. This stimulates the production of collagen cells, which are needed to repair the damage and help MCL injuries.
As prolotherapy treats the root cause of MCL Injuries, it is considered a permanent fix, preventing symptoms from returning.
Disclaimer: The information provided in this section is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Prolotherapy may not be suitable for everyone, and outcomes can vary. Always seek the guidance of a qualified healthcare professional regarding your specific medical condition or treatment options. Never disregard professional medical advice or delay seeking it because of information you have read here.
Frequently Asked Questions
How long does it take an MCL injury to heal?
Grade 1 injuries may heal in a few days to a week, grade 2 in 2–4 weeks, and grade 3 may take several weeks to months, depending on severity and treatment.
Can you walk with an MCL injury?
Walking is possible with minor MCL injuries, but severe injuries may cause instability and pain, limiting mobility until healing occurs.
How do you tell if MCL is torn or sprained?
A healthcare professional will assess your knee’s stability and pain during a physical exam, sometimes using imaging to confirm a tear or sprain.
Which is worse, ACL or MCL tear?
ACL tears are generally more severe, harder to treat, and have a longer recovery time than MCL tears.
Is walking good for torn ligaments?
Walking may be recommended after pain and swelling subside, but avoid overuse and follow your doctor’s advice.
How do you sleep with a torn MCL?
Use a pillow between your knees for support, sleep on your back or side with knees slightly flexed, and avoid crossing your legs.
Contact ProHealth Clinic Today for Your FREE 15-Minute Discovery Call
Don’t let MCL Injuries control your life any longer. Join the thousands of patients who have found lasting relief through prolotherapy at ProHealth Clinic.
Get in Touch
Phone: +441234380345
Email: info@prohealthclinic.co.uk
Our Clinic Locations
London: 104 Harley Street, Marylebone, W1G 7JD
Manchester: The Hadley Clinic, 64 Bridge Street, M3 3BN
Bedford: The Village Medical Centre, Kingswood Way, MK40 4GH
All clinics offer the same award-winning prolotherapy treatment with convenient appointment times, including evenings and weekends.
References
- Desai, V. S., et al. (2020). The journal of knee surgery, 33(8), 785–791.
- Loughran, G. J., et al. (2019). The American journal of sports medicine, 47(6), 1294–1301.
- Lundblad, M., et al. (2019). Knee surgery, sports traumatology, arthroscopy, 27(11), 3692–3698.
- Elkin, J. L., et al. (2019). Current reviews in musculoskeletal medicine, 12(2), 239–244.
- Jung, K. H., et al. (2019). Arthroscopy, 35(5), 1520–1524.
- Westermann, R. W., et al. (2019). Arthroscopy, 35(5), 1466–1472.
- Albtoush, O. M., et al. (2019). Clinical imaging, 53, 32–34.
- DeFroda, S. F., et al. (2019). The Physician and sportsmedicine, 47(1), 129–131.
- Encinas-Ullán, C. A., & Rodríguez-Merchán, E. C. (2018). EFORT open reviews, 3(7), 398–407.
- Goff, A. J., et al. (2018). Physical therapy in sport, 34, 227–237.
- Logan, C. A., et al. (2018). Orthopaedic journal of sports medicine, 6(7), 2325967118787182.
Disclaimer: This article is for informational purposes only and does not substitute for professional medical advice. Always consult your healthcare provider before making treatment decisions.