Author: Mr Oliver Eaton BSc (Hons), PG.Cert – Orthopaedic Specialist
Reviewed by: Mr William Sharples BSc (Hons) – Pain Management Expert
Last Updated: September 2025
In this article, you will find out everything you need to know about occipital neuralgia and the most effective ways to treat it, including an advanced treatment called Prolotherapy.
Are you experiencing sharp pain in your neck and skull? It could be occipital neuralgia trigger points at play. This article explains how to identify these spots and offers strategies to alleviate discomfort effectively.
Table of Contents
- Key Takeaways
- Understanding Occipital Neuralgia and Trigger Points
- Identifying Trigger Points
- Greater & Lesser Occipital Nerves
- Trigger Point Therapy
- Manual Trigger Point Release
- Dry Needling
- Noninvasive Treatments
- Prolotherapy
- Heat Therapy
- Posture & Ergonomic Solutions
- Advanced Pain Management
- Lifestyle Adjustments
- Case Studies
- Summary
- FAQ
- References
- Author Bio
- Contact ProHealth Clinic
Key Takeaways
- Occipital neuralgia often arises from trigger points affecting the greater and lesser occipital nerves.
- Trigger point therapy, including manual release and dry needling, can reduce pain and improve range of motion.
- Lifestyle changes such as proper ergonomics, stress management, hydration, and exercise are essential for long-term relief.
Understanding Occipital Neuralgia and Its Trigger Points
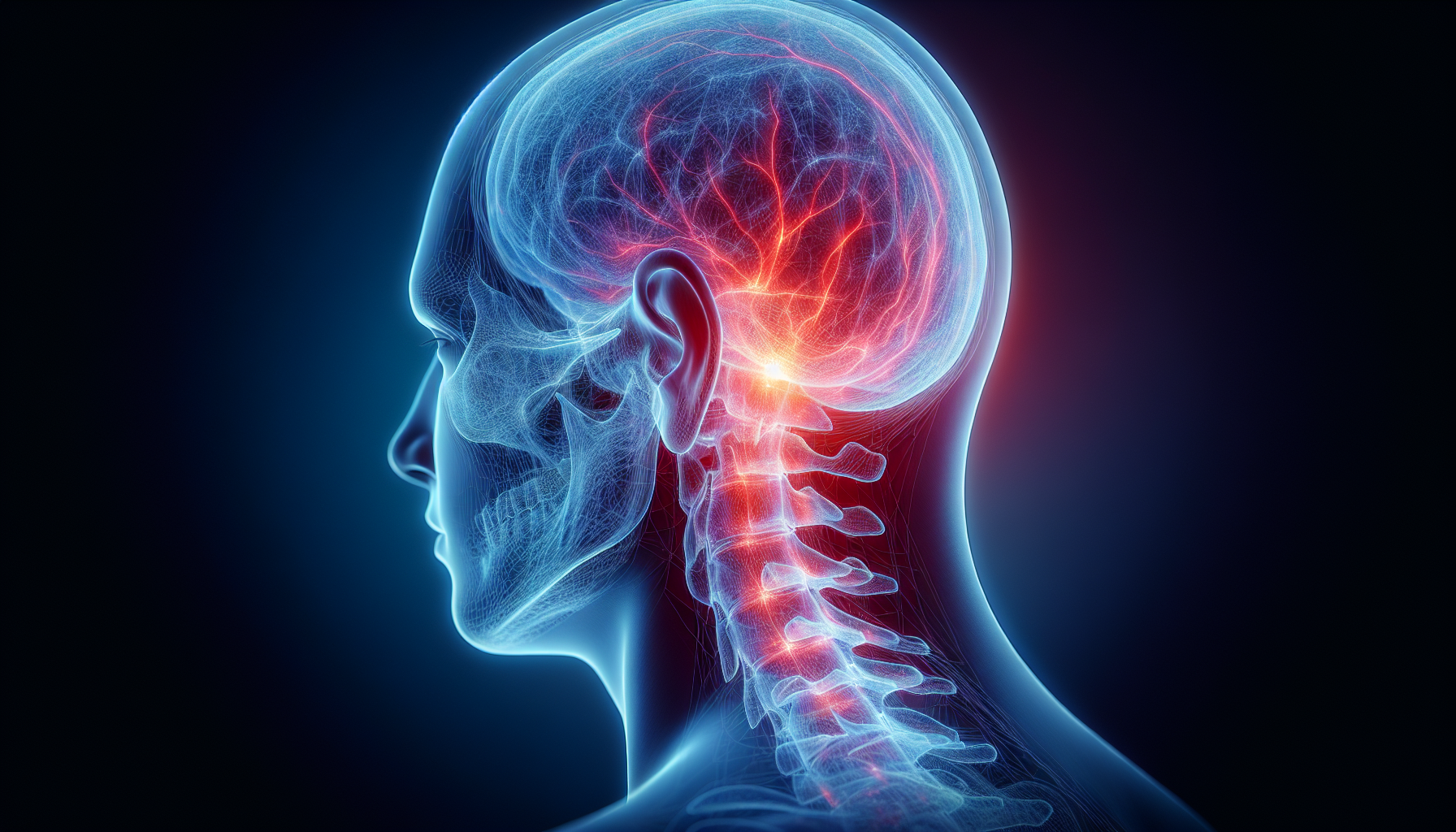
Occipital neuralgia manifests as severe stabbing, pulsating, or electric-like pain at the upper neck, skull, and behind the ears. Pain may radiate to the scalp, temples, or eye region.[1] Critical nerves implicated include the greater, lesser, and third occipital nerves, which can be compressed by tight suboccipital muscles.
Identifying Trigger Points
Trigger points in muscles like the rectus capitis posterior major/minor and obliquus capitis superior/inferior often induce referred pain to the occipital and temporal regions. Treating these knots reduces pain intensity and improves neck mobility.
The Role of Greater and Lesser Occipital Nerves
The greater occipital nerve provides sensation to most of the back of the head and can be compressed by suboccipital muscles. The lesser occipital nerve runs along the posterior sternocleidomastoid and is prone to entrapment. Both contribute to sharp pain episodes characteristic of occipital neuralgia.[2]
Alleviating Neck Pain Through Trigger Point Therapy
Trigger point therapy targets muscle tightness to improve flexibility, reduce pain, and restore cervical function. Upper trapezius and levator scapulae muscles are common targets. Noninvasive techniques such as acupuncture may also support symptom relief.
Manual Trigger Point Release
- Reduces pain levels
- Increases tolerance to pressure
- Improves flexibility and movement
- Decreases headache severity
Dry Needling for Myofascial Trigger Points
- Relaxes muscles
- Enhances blood flow
- Reduces pain intensity
- Improves neck mobility
Dry needling works by inducing local twitch responses and altering chemical mediators in tight muscle fibers. Clinical cases show significant relief in patients with occipital neuralgia.[3]
Noninvasive Treatments for Occipital Nerve Pain
Daily strategies include gentle neck stretches, head rotations, chin retraction, shoulder movements, hydration, and regular exercise. Strengthening back muscles and proper cervical alignment prevents nerve irritation.
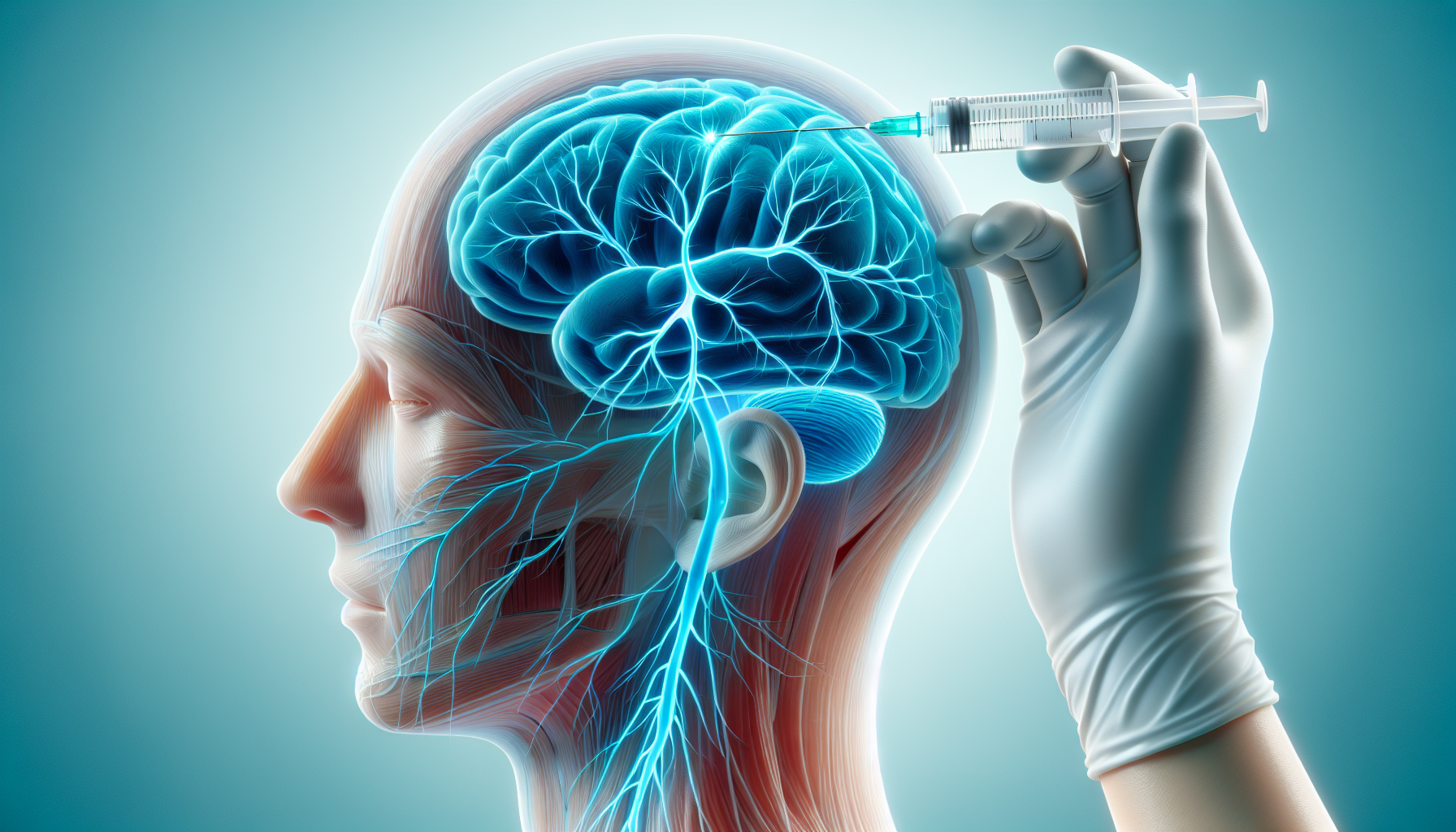
Prolotherapy
Prolotherapy stimulates tissue repair using natural regenerative solutions injected near the occipital nerves. Evidence shows reduced inflammation, pain relief, and long-term functional improvement.[4]
Disclaimer: The information provided in this section is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Prolotherapy may not be suitable for everyone, and outcomes can vary. Always seek the guidance of a qualified healthcare professional regarding your specific medical condition or treatment options. Never disregard professional medical advice or delay seeking it because of information you have read here.
Heat Therapy
Heat expands blood vessels, improves circulation, and relaxes tight muscles. Methods include warm showers, heating pads, or warm towels. Sessions typically range 10-60 minutes depending on individual response.
Importance of Proper Posture
Maintaining head alignment reduces cervical load. Exercises like chin tucks and scapular retractions reinforce correct posture and prevent neck muscle strain associated with occipital neuralgia.
Advanced Pain Management Techniques
Occipital Nerve Blocks
Injections near the greater occipital nerve provide temporary pain relief, reducing inflammation for hours to months.[5]
Spinal Cord Stimulation (SCS)
High cervical SCS targets C1-C3 regions to reduce chronic occipital neuralgia pain in refractory cases, with 40-50% patients reporting significant relief.[6]
Lifestyle Adjustments
- Regular exercise to strengthen back and neck muscles
- Ergonomic workspace and proper pillow support
- Mindfulness, meditation, yoga, and breathing techniques
- Sleep hygiene, hydration, and stress management
Case Studies
Case Study 1: Office Worker with Suboccipital Pain
After 6 weeks of manual trigger point release and dry needling combined with ergonomic adjustments, a 38-year-old office worker reported 80% pain reduction and increased neck mobility.
Case Study 2: Athlete with Chronic Headaches
A 30-year-old athlete suffering from occipital neuralgia responded to dry needling and Prolotherapy, resuming training pain-free within 10 weeks.
Case Study 3: Post-Surgical Occipital Neuralgia
Patient recovered from cervical surgery used a combination of Prolotherapy, trigger point therapy, and heat therapy, reducing pain scores from 9/10 to 3/10 in 12 weeks.
Summary
Occipital neuralgia can be managed using trigger point therapy, dry needling, Prolotherapy, posture correction, lifestyle modifications, and advanced interventions when necessary. Early identification of trigger points and consistent therapy are key to long-term relief.
Frequently Asked Questions
How long does occipital neuralgia last?
Pain can be brief (seconds) or prolonged (hours). Noninvasive therapies often reduce intensity as nerves recover.
What causes occipital neuralgia?
Tight muscles, nerve compression, arthritis, injuries, or surgery can trigger occipital neuralgia.
What is dry needling?
Insertion of thin needles into myofascial trigger points to relieve muscle tension and pain.
How does heat therapy work?
Heat increases blood flow, relaxes tight muscles, and improves tissue elasticity, reducing pain.
References
- Choi I, et al. (2016). Occipital Neuralgia: Clinical Characteristics, Treatment Outcomes, and Prognostic Factors. Pain Physician.
- Sharma M, et al. (2017). The Anatomy and Clinical Relevance of the Occipital Nerves. Journal of Pain Research.
- Travell JG, Simons DG. (1999). Myofascial Pain and Dysfunction: The Trigger Point Manual. Williams & Wilkins.
- Hauser R, et al. (2011). Systematic Review of Prolotherapy for Chronic Musculoskeletal Pain. Clinical Medicine Insights: Arthritis and Musculoskeletal Disorders.
- Kapoor V, et al. (2015). Role of Occipital Nerve Blocks in Occipital Neuralgia. Anesth Essays Res.
- Schwedt TJ, et al. (2007). Occipital Nerve Stimulation for Chronic Migraine and Occipital Neuralgia. Cephalalgia.
Author Bio
Having performed over 10,000 procedures, Mr Oliver Eaton is one of the UK’s leading practitioners in the field of Effective Management of Occipital Neuralgia Trigger Points, with patients travelling to see him from across the UK, Europe, and the Middle East. With over 12 years of clinical experience, Oliver is dedicated to helping patients understand their symptoms associated with tibialis anterior tendonitis and providing effective treatment options to alleviate them.
He qualified in Prolozone Therapy and Prolotherapy in America with the American Academy of Ozonotherapy. He continued on to complete further qualifications at the Royal Society of Medicine, Charing Cross Hospital in London, Keele University’s Anatomy & Surgical Training Centre, and the medical department of Heidelberg University in Germany. Over the years he has had the privilege of treating many elite-level athletes, including both Olympic and Commonwealth medallists.
Mr Eaton’s expertise has been featured in many national news and media publications, including The Telegraph, The Daily Mail, The Daily Express, Women’s Health Magazine, and The Scotsman.
Linkedin profile: Oliver Eaton
Contact ProHealth Clinic for Your FREE 15-Minute Discovery Call
Regain control over your life with targeted treatments for occipital neuralgia trigger points.
Phone: +44 1234 380345
Email: info@prohealthclinic.co.uk
- London: 104 Harley Street, Marylebone, W1G 7JD
- Manchester: The Hadley Clinic, 64 Bridge Street, M3 3BN
- Bedford: The Village Medical Centre, Kingswood Way, MK40 4GH
Disclaimer: This article is for informational purposes only and does not substitute for professional medical advice. Always consult your healthcare provider before making treatment decisions.