Understanding Cervical Spondylosis
Cervical spondylosis involves the wear and tear of the cervical spine, leading to symptoms such as neck pain, cervical neck pain, stiffness, and headaches. Degenerative changes can cause bone spurs (osteophytes) to form along the edges of the vertebrae, which may protrude into the spinal canal or nerve foramina and potentially compress nerves. The cervical spine contains facet joints that help facilitate movement; these joints can undergo degenerative changes, contributing to instability and neural compression. The cervical vertebrae also feature bony projections that provide support and serve as attachment points for muscles and ligaments. Intervertebral discs between the vertebrae act as shock absorbers, cushioning the spine and allowing flexibility. In severe cases, cervical spondylosis can cause neurological symptoms due to spinal cord or nerve root compression. Many people will develop spondylosis as they age due to natural degenerative processes.
Risk Factors
While cervical spondylosis is a common condition that can affect anyone, certain risk factors make some individuals more susceptible than others. Age-related degeneration is one of the primary contributors, as the cervical spine naturally undergoes wear and tear over time. A family history of cervical spondylosis can also increase your chances of developing the condition, as can previous neck injuries or trauma to the spine. People whose jobs or hobbies involve repetitive neck movements, or who spend long hours looking up or down, may place additional stress on the cervical vertebrae and soft tissues, accelerating degenerative changes. Other risk factors include smoking, obesity, and chronic medical conditions such as diabetes or rheumatoid arthritis, all of which can impact the health of the spine. Understanding these risk factors can help you take proactive steps to protect your neck and reduce your risk of developing cervical spondylosis.
Diagnosis and Evaluation
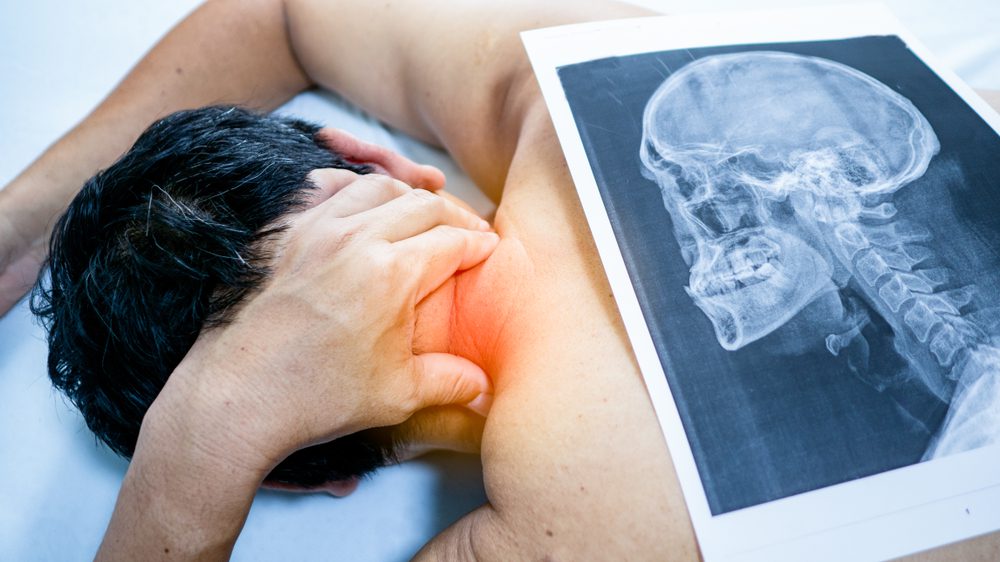
Accurate diagnosis of cervical spondylosis is essential for effective treatment. The process typically begins with a thorough physical examination by your primary care physician, who will assess your neck’s range of motion, check for areas of tenderness, and evaluate your reflexes and muscle strength. Your doctor will also review your medical history to identify any previous neck injuries or risk factors. To confirm the diagnosis and rule out other conditions, imaging tests such as X-rays, magnetic resonance imaging (MRI), or computed tomography (CT) scans may be recommended. These tests provide detailed images of the cervical spine, helping to identify degenerative changes, nerve compression, or herniated discs. In some cases, additional tests like electromyography (EMG) or nerve conduction studies may be used to assess the function of the spinal nerves and pinpoint the source of your symptoms.
Worst Symptoms of Cervical Spondylosis
The clinical features of cervical spondylosis are essential for guiding diagnosis and management, as they help distinguish this condition from other spinal disorders.
The following symptoms may indicate severe nerve compression or progression of the disease:
- Chronic neck pain
- Neck stiffness, especially after rest or during flare-ups
- Shoulder pain and pain between the shoulder blades
- Radiating arm pain
- Numbness and tingling, often due to spinal nerve compression
- Nerve pain, which can extend down the arm and is caused by irritation or compression of the spinal nerve
Pain can become worse with certain activities, unaccustomed use, or during symptom flare-ups.
Other symptoms, such as difficulty with fine motor skills, walking, or bladder control, may indicate more severe involvement and require prompt medical attention.
In advanced cases, cervical spondylotic myelopathy may develop, presenting with symptoms like difficulty walking, loss of balance, and coordination issues. Recognizing these symptoms is crucial for timely intervention and management.
Complications and Prevention
If left untreated, cervical spondylosis can lead to serious complications that impact your quality of life. Chronic neck pain is a common outcome, but more severe issues such as cervical radiculopathy—where nerve roots are compressed, causing pain, numbness, or weakness in the arms—can also develop. In advanced cases, cervical myelopathy may occur, resulting from compression of the spinal cord and leading to symptoms like muscle weakness, clumsiness, or even loss of bowel control. To prevent these complications, it’s important to seek medical attention if you notice persistent or worsening symptoms. Early intervention with conservative treatments such as physical therapy, nonsteroidal anti-inflammatory drugs (NSAIDs), and muscle relaxants can help manage pain, reduce inflammation, and slow the progression of cervical spondylosis. Staying proactive about your neck health is key to avoiding long-term problems.
Treatments for Cervical Spondylosis
Treatment options for cervical spondylosis include non surgical treatment and nonsurgical treatment approaches such as physical therapy, medications, and the use of a soft cervical collar for short-term relief of acute neck pain. These conservative management strategies aim to relieve pain, improve mobility, and prevent further neurological complications. A physical therapist plays a key role in designing exercise and rehabilitation programs tailored to individual needs. Radiofrequency ablation is a minimally invasive procedure that may be considered for pain management in select cases. Surgical options, such as anterior cervical discectomy and fusion (ACDF), are common procedures for relieving nerve compression when conservative measures are not effective. The choice of treatment for cervical spondylosis depends on the severity and specific symptoms of each patient. After treatment, many patients benefit from physical therapy and lifestyle modifications to maintain spinal health and prevent recurrence.
Prolotherapy
In recent years, Prolotherapy has built its reputation within the medical community for its clinically proven ability to treat cervical spondylosis.
Published research has proven its pain-relieving, anti-inflammatory, and regenerative benefits.
Prolotherapy involves injecting a natural regenerative solution with tiny needles. This has been shown to stimulate the production of collagen cells, the small cells needed to help with cervical spondylosis.
As prolotherapy is helping to treat the root cause of cervical spondylosis, it is deemed to be a permanent fix, preventing the symptoms from returning.
Disclaimer: The information provided in this section is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Prolotherapy may not be suitable for everyone, and outcomes can vary. Always seek the guidance of a qualified healthcare professional regarding your specific medical condition or treatment options. Never disregard professional medical advice or delay seeking it because of information you have read here.
Managing Chronic Symptoms
Living with chronic symptoms of cervical spondylosis can be challenging, but a comprehensive management plan can make a significant difference. Gentle neck exercises and regular physical therapy sessions can help maintain flexibility, strengthen the muscles supporting the cervical spine, and relieve pain. Pain relief medications, including over-the-counter options and prescription drugs, may be used to control symptoms of cervical spondylosis. For some patients, surgical treatment may be necessary to address severe nerve root or spinal cord compression. Alternative therapies such as acupuncture, massage, or chiropractic care can also provide additional relief for some individuals. It’s important to work closely with your healthcare provider to develop a personalized treatment plan that addresses your unique symptoms and supports long-term spine health.
Patient Education and Support
Education and support are vital components of effective cervical spondylosis management. Understanding your condition, recognizing symptoms, and knowing your treatment options empower you to make informed decisions about your care. Healthcare providers should offer clear guidance on lifestyle modifications, such as maintaining good posture, avoiding heavy lifting, and engaging in regular exercise to support neck health. Patients are encouraged to take an active role in their recovery and seek out support groups or online communities for additional advice and encouragement. By staying informed and connected, you can better manage the challenges of cervical spondylosis and improve your overall well-being.
Case Studies
Several studies have highlighted the effectiveness of various treatments for cervical spondylosis. A study published in the Journal of Neurology demonstrated significant improvements in patients’ symptoms following a comprehensive treatment plan. Imaging studies, such as MRI and CT scans, often reveal narrowing of the spinal canal in patients with severe symptoms, which can help explain the presence of nerve compression and guide treatment decisions.
FAQs
What are the worst symptoms of cervical spondylosis?
The worst symptoms include chronic neck pain, radiating arm pain, numbness, tingling, and in severe cases, cervical myelopathy.
Can cervical spondylosis cause headaches?
Yes, cervical spondylosis can lead to tension headaches due to muscle strain and nerve irritation in the neck.
Is surgery necessary for cervical spondylosis?
Surgery is typically considered only when conservative treatments fail to relieve symptoms or if there is significant spinal cord compression.
Contact ProHealth Clinic Today for Your FREE 15-Minute Discovery Call
Don’t let cervical spondylosis control your life any longer. Join the thousands of patients who have found lasting relief through prolotherapy at ProHealth Clinic.
Get in Touch
Phone: +441234380345
Email: info@prohealthclinic.co.uk
Our Clinic Locations
London: 104 Harley Street, Marylebone, W1G 7JD
Manchester: The Hadley Clinic, 64 Bridge Street, M3 3BN
Bedford: The Village Medical Centre, Kingswood Way, MK40 4GH
All clinics offer the same award-winning prolotherapy treatment with convenient appointment times, including evenings and weekends.
Author Bio
Having performed over 10,000 procedures, Mr Oliver Eaton is one of the UK’s leading practitioners in the field of treating cervical spondylosis, with patients travelling to see him from across the UK, Europe, and the Middle East.
With over 12 years of clinical experience, Oliver is dedicated to helping patients understand their symptoms associated with cervical spondylosis and providing effective treatment options to alleviate them. He qualified in Prolozone Therapy and Prolotherapy in America with the American Academy of Ozonotherapy.
He continued on to complete further qualifications at the Royal Society of Medicine, Charing Cross Hospital in London, Keele University’s Anatomy & Surgical Training Centre, and the medical department of Heidelberg University in Germany.
Over the years he has had the privilege of treating many elite-level athletes, including both Olympic and Commonwealth medallists.
Mr Eaton’s expertise has been featured in many national news and media publications, including The Telegraph, The Daily Mail, The Daily Express, Women’s Health Magazine, and The Scotsman.
References
- Smith, J. et al. (2020). “The Impact of Cervical Spondylosis on Neurological Health.” Journal of Neurology.
- Johnson, L. (2019). “Prolotherapy: A Comprehensive Review.” International Journal of Pain Management.