Platelet-rich plasma therapy (PRP) is a simple outpatient procedure that helps to enhance the natural growth factors your body uses to heal tissue. We describe the difference between PRP injections and the more advanced Prolotherapy injections in this article.
Prolotherapy involves the injection of a dextrose solution into an injured, weak or degenerated part of the body. This helps to stimulate the production of fibroblasts. Fibroblasts help to secrete the collagen needed to repair and strengthen damaged or degenerated body tissue. The injected substance is very fine so it has the ability to spread into the injured area much more effectively than platelet-rich plasma injections. The below video is a collection of testimonials of our patients that have received Prolotherapy at our clinic.
PRP injections are a preparation of autologous human body plasma, consisting of a concentration of platelets. This concentration of platelets contains a rich deposit of growth factors stored as alpha granules.
Once the platelets have been activated they help to support cell growth and repair. Primarily, they augment the natural process of soft tissue healing and recovery time of sports injuries such as tennis elbow, pulled hamstring muscles, knee sprains and jumper’s knee. It also might be affective for chronic tendon injuries, like those affecting the patellar tendon. In a normal blood sample, the platelet count ranges between 150,000 to 350,000 per mililitre. At a concentration of above 1,000,000 per mililitre, improved tissue healing and bone regeneration have been recorded.
Platelet-Rich Plasma: Preparation and Composition
The core principle of PRP treatments is generally similar.
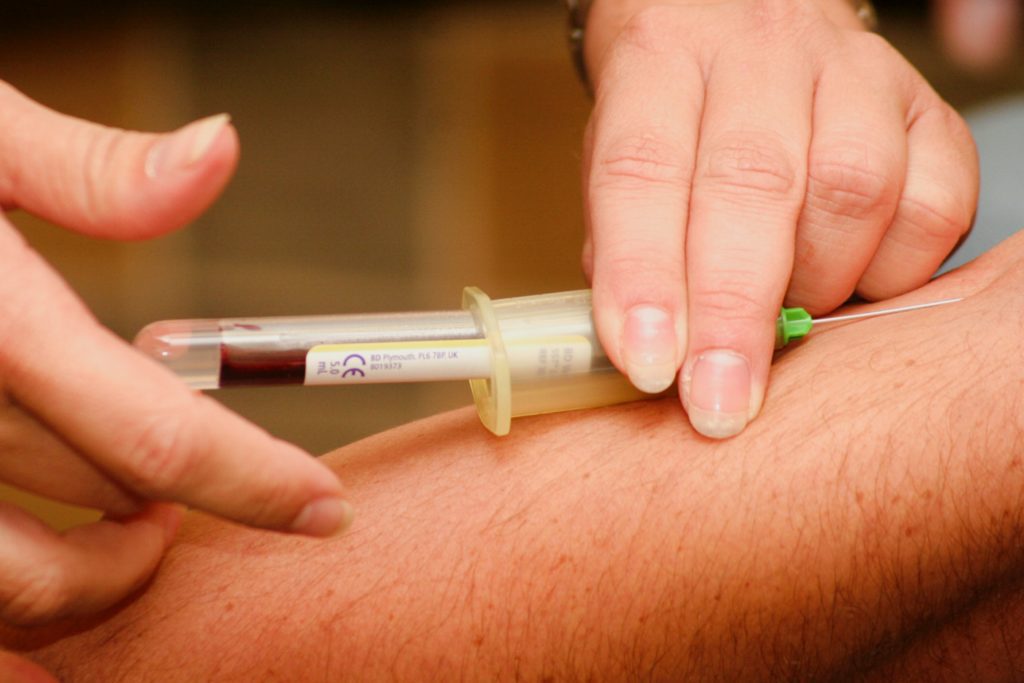
The PRP therapy formulation procedure starts with the collection of whole blood samples from the patient. After collection of the patients own blood, the blood sample is then mixed with an anticoagulant factor in a centrifuge. Centrifugation is done at a varying speed until the blood separates out into three distinct layers. The three layers consist of the platelet-poor blood, red blood cells (RBC), and a buffy layer of concentrated leucocytes (white blood cells) and concentrated platelets.
The centrifuge separates the red blood cells from platelet-rich plasma. The concentrated platelet layer is then separated using different isolation methods, at least triple the concentration of the blood sample. The platelet-rich plasma layer can be directly injected into musculoskeletal injury sites or activated with a platelet activator to speed up the healing process. Activation immediately de-granulates the platelets and trigger the release of growth factors, stem cells and a bioactive substance involved in regenerative tissue healing. It is important to remember that this is a safe natural procedure as it involves a patients own blood taken from their own body (autologous).
Application of Platelet-Rich Plasma in Medicine
- Treatment of Muscle Injury
This is perhaps the most popular indication of platelet-rich plasma injections in sports medicine. The biological processes involved in muscle repair start with local inflammatory response and end with cell proliferation, differentiation, tissue repair and tissue remodelling. Many clinical studies and orthopaedic assessments have produced convincing evidence suggesting that a supervised PRP injection regimen speeds up the healing process.
- PRP Injection for tendon problems and acute sports injuries
PRP injections have long been proposed as supportive therapy in the treatment of torn tendon and tendonitis in healthcare. They are a much safer alternative to cortisone. The cytokines released by the concentrated volume of platelets in these injections are involved in the healing stage of tendinopathies such as golfer’s elbow. The substances released at the injection site also promote vascularization of the injury site –an action that directly improves blood and nutrient supply to the healing tissue. In chronic tendon injuries, multiple PRP injections might be required for healing tendonitis. Reports from various clinical trials have shown evidence supporting the use of ultrasound guidance with PRP in the management of Achilles tendinopathy, lateral epicondylitis, patellar tendinopathy, plantar fasciitis, and rotator cuff tendinopathy.
- Surgical Augmentation
PRP injections are theoretically useful in promoting regenerative tissue healing and cell differentiation. Orthopaedic surgeons used a platelet-rich fibrin matrix for surgical augmentation in these studies. PRP formulations directly injected into the injury sites releases abundant growth factors and cytokines that speeds up the healing process. As it stands, there is evidence supporting the use of PRP in rotator cuff repair, Achilles tendon repair, and anterior cruciate ligament surgery.
Numerous Pilot Study evaluating PRP injections have also been reported to be beneficial in the management of other musculoskeletal conditions, including ankle sprains, osteoarthritis, and fractures. The release of multiple growth factors by PRP injections are a major advantage over single recombinant human growth factor delivery formulations. There are many peer reviewed studies and synchronous observational cohort studies currently investigating how orthopaedic surgeons efficiently combined PRP with surgery as an advanced therapy approach for patients in need of rapid bone and muscle regeneration.
Frequently Asked Questions –
How long do PRP injections last?
The full effect of the injection can take up to several months to be felt. As the aim of the treatment is to repair, the effect is often lasting. Maximum results are normally achieved at between 6-9 months.
Is PRP treatment painful?
PRP injections do not usually cause pain. Any pain experienced around the injection site is only temporary. The site of the injection is thoroughly numbed before the injection to ensure maximum comfort and minimum pain during the procedure.
What is the success rate of PRP injections?
The success rate depends on the condition or injury being treated. On average, PRP treatment has an 80% success rate.
How many PRP injections are needed?
One to three injections are required to achieve optimum results. As stated above, a follow-up may be required for conditions such as knee osteoarthritis.
How often should Platelet Rich Plasma (PRP) injections be given?
The liquid portion found at the top of the syringe, also known as liquid gold is injected after one months intervals. It is advised not to take a several weeks long gap between the treatment sessions and one month is ideal to improve healing for tissue damage and treat health conditions like jumpers knee, and injuries after special surgery.
Can you walk after Platelet Rich Plasma (PRP) injection?
It is a simple outpatient procedure so you are able to walk after the injections, although it is not advised to walk more than you would normally walk in a day.
Is Platelet Rich Plasma (PRP) good for arthritis?
PRP treatment has shown to be effective for mild to moderate osteoarthritis. It can still be effective for severe arthritis but only if it is combined with a tailored exercise program to strengthen the muscles around the knee. This is something we provide at our clinic alongside the injections. PRP is a much safer alternative to cortisone. The medical department of Boston University published an article in 2019 highlighting the dangers of cortisone for hip and knee osteoarthritis.
Can I take painkillers after the procedure?
It is okay to take paracetamol but not anti-inflammatory medications such as ibuprofen. The doctor may be advised about question about other medications. Not many individuals report symptoms of pain after a prp procedure. As the platelet rich plasma (PRP) is injected directly to the skin surface via fine needles, some doctors with relevant experience may also not use local anesthetic.
Are there potential side effects associated with PRP therapy?
The only main side effect associated with PRP treatments is soreness that can last up to a week. There is also less chances of adverse reactions and allergic reaction, as the patients own plasma and blood cell is being used.
Can platelet-rich plasma (PRP) be used for any other conditions?
PRP injections are a common treatment to promote hair growth in patients with hair loss due to male pattern baldness. It may also be effective for hair loss associated with alopecia. Hair growth is a big industry. Autologous platelet treatment may also be recommended by wellness professionals for treating degenerative tendinopathies due to its wound healing properties. According to a randomized control trial, it may also be effective for Knee osteoarthritis.
Can I still perform physiotherapy exercises after the treatment?
It is still okay to perform gentle non-weight bearing physiotherapy exercises prescribed by a medical professional or physiotherapist after platelet-rich plasma treatment. These can be effective for muscle injuries, injured tendons and tennis elbow.
Are there contraindications?
We do not advise individuals with blood clotting problems to have the treatment. Moreover, it is best to consult a healthcare professional in case of any concerns and questions.
IS PRP covered by Medical Insurance?
Cosmetic Procedures like PRP is not usually covered by insurance plans, since it is still at an experimental stage. Moreover, it is also recommended that every patient going for their treatment should check the background of the doctor and their training before hand, for preventing fraud. They should particularly be vary of this during booking sessions ; the patients should securely process their payments and manage settings of their online banking system.
This procedure is commonly promoted on Healthline media websites and other sources of healthline media as an invaluable service and as a means to grow more hair.